What are Gram-negative bacilli? Structure and significance in Gram staining?
What are Gram-negative bacilli?
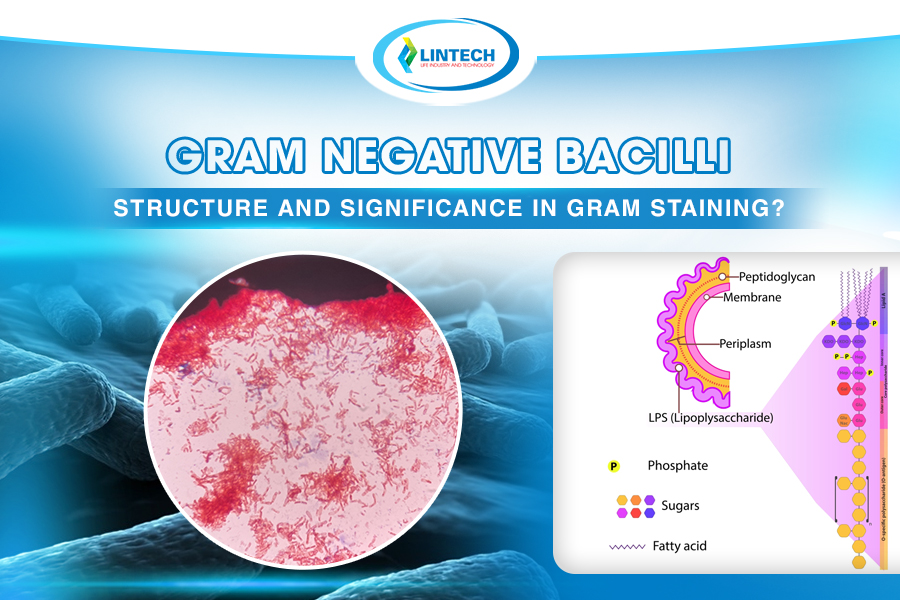
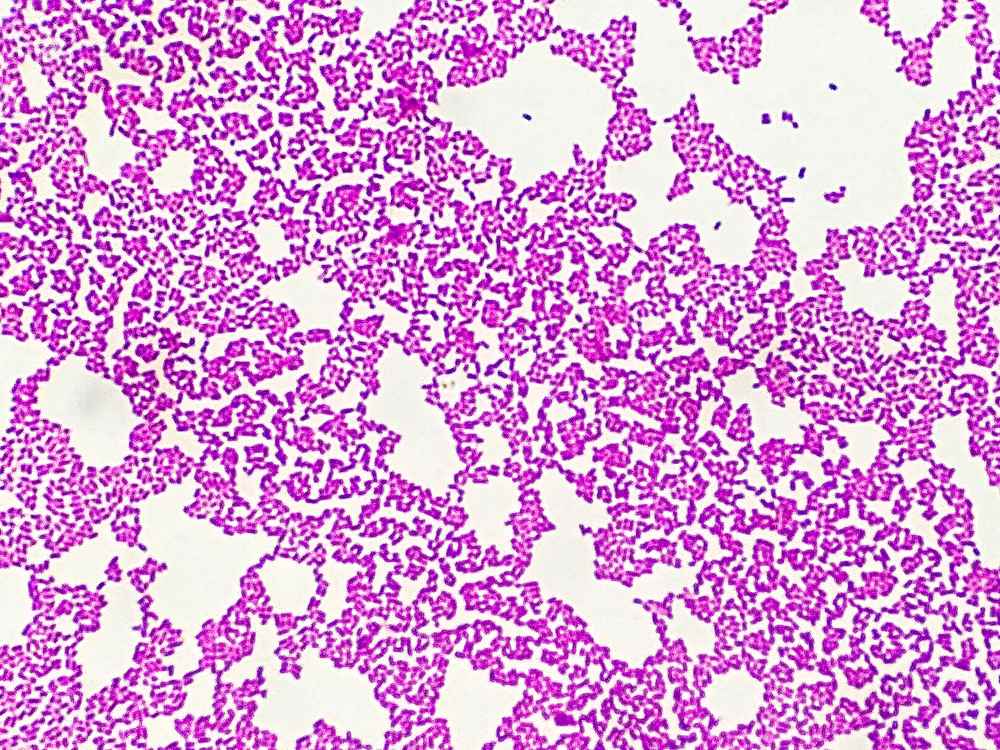
Gram-negative bacilli are rod-shaped bacteria (straight or slightly curved) that belong to the Gram-negative group according to the Gram staining classification. When stained using the Gram method, they appear pink or red under the microscope.
Gram-negative bacilli are widely present in natural environments such as soil, water, the human and animal digestive systems, as well as in hospital settings. They can become pathogenic agents when the body’s immune system is weakened or when favorable conditions exist, such as open wounds, invasive medical procedures, or poor hygiene.
During staining, Gram-negative bacteria do not retain the crystal violet purple color; they are decolorized by alcohol and then take up the red or pink color from safranin. This characteristic reflects a thinner cell wall with less peptidoglycan and an outer membrane containing lipopolysaccharide (also called endotoxin), which triggers strong inflammatory responses in the human body.
Gram-negative bacilli are divided into two main groups
Group of sugar-fermenting Gram-negative bacilli:
Typically belong to the Enterobacteriaceae family, capable of fermenting glucose to produce energy.
Typical representatives include
Escherichia coli coliform bacillus, Klebsiella pneumoniae pneumonia bacillus, Salmonella typhoid bacillus, Shigella bacillary dysentery. This group commonly causes infections in the gastrointestinal tract, urinary tract, and bloodstream.
Group of non-sugar-fermenting Gram-negative bacilli:
They do not ferment glucose but only oxidize it. Common types include Pseudomonas aeruginosa (blue-green pus bacillus), Acinetobacter baumannii, Burkholderia cepacia, Stenotrophomonas maltophilia.
This group often causes hospital-acquired infections, especially in immunocompromised patients, with an isolation rate of approximately 12 percent among all pathogenic bacteria according to recent studies.
Gram-negative bacilli are not only pathogenic bacteria; some are also normal components of the microbiota in the body, such as in the intestines or female genital tract. However, when imbalance occurs, they can lead to serious infections.
Cell structure of Gram-negative bacilli
The cell structure of Gram-negative bacilli is quite complex and different from Gram-positive bacteria, contributing to their antibiotic resistance and pathogenicity. Specifically:
- Nucleus of Gram-negative bacilli: No true nucleus, but a nucleoid region containing a single circular DNA molecule without a surrounding membrane.
- Cytoplasm: Contains ribosomes, enzymes, and essential nutrients for life.
- Cytoplasmic membrane: Lipid bilayer layer that controls metabolism and transport.
- Cell wall: Thinner than in Gram-positive bacteria, with a thin peptidoglycan layer (about 10 percent of the cell wall), high lipid content and
- no teichoic acid. This layer determines the Gram-negative characteristic.
- Outer membrane: Characteristic of Gram-negative bacteria, containing lipopolysaccharide endotoxin that causes fever and septic shock. There is a periplasmic space between the outer membrane and cytoplasmic membrane, containing hydrolytic enzymes.
- Capsule: Outer polysaccharide layer that helps bacteria adhere and evade the immune system.
- Pili and fimbriae: Structures that aid movement, adhesion to cells, and gene exchange such as sex pili.
- Flagella: Some types have flagella for motility, such as Pseudomonas aeruginosa.
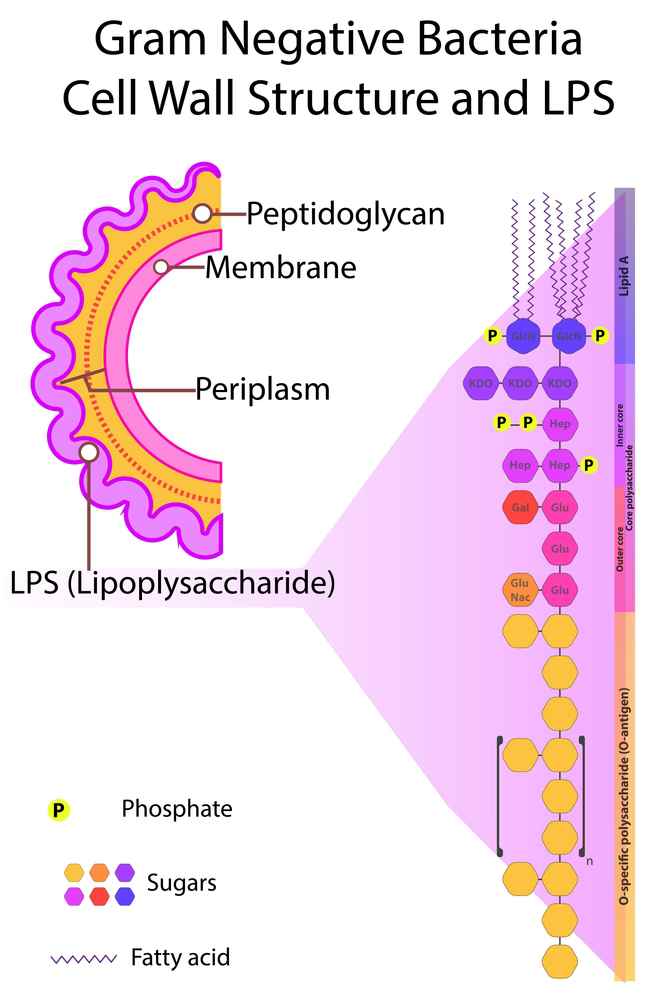
This structure makes Gram-negative bacilli resistant to penicillin due to thin peptidoglycan but sensitive to some other antibiotics, while the endotoxin causes strong inflammatory responses.
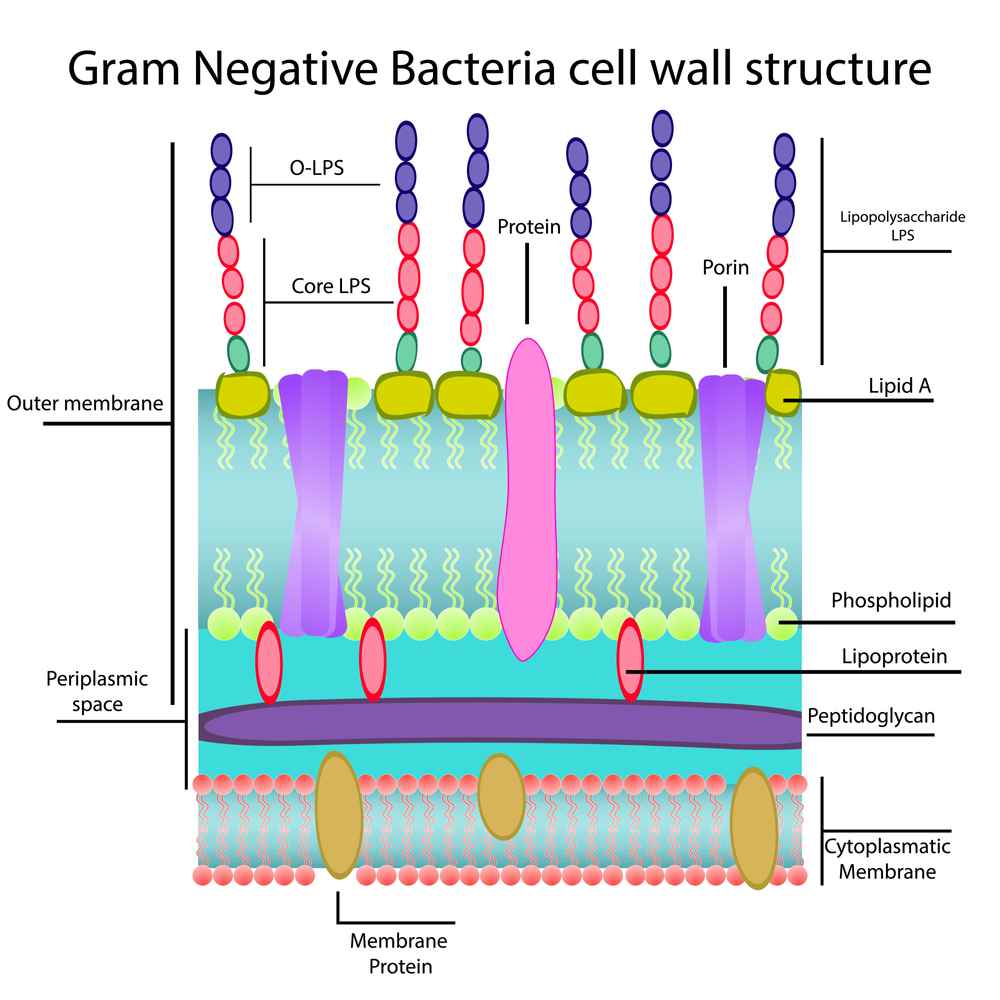
Common types of Gram-negative bacilli and their pathogenic roles
There are hundreds of types of Gram-negative bacilli, but the most common include:
- Pseudomonas aeruginosa (blue-green pus bacillus): Present in water, soil, and hospital environments. Causes wound infections, otitis externa, keratitis, ventilator-associated pneumonia, urinary tract infections, and bloodstream infections in immunocompromised individuals.
- Acinetobacter baumannii: Common in hospitals, causes hospital-acquired pneumonia and bloodstream infections with high resistance rates (>70%) to many antibiotic groups.
- Escherichia coli (coliform bacillus): Normal intestinal flora, causes diarrhea, urinary tract infections, peritonitis, and sepsis.
- Klebsiella pneumoniae: Causes pneumonia, urinary tract infections, and sepsis.
- Salmonella: Causes typhoid fever and diarrhea from contaminated food.
- Shigella: Causes bacillary dysentery with bloody and mucoid diarrhea.
- Other types: Burkholderia cepacia causes infections in cystic fibrosis patients, Stenotrophomonas maltophilia causes respiratory infections, Yersinia pestis causes plague, Vibrio cholerae causes cholera, Bordetella pertussis causes whooping cough.

These bacteria are commonly found in the environment and become dangerous when they enter through skin, mucous membranes, respiratory, or digestive routes.
Gram staining method and mechanism for distinguishing Gram-negative bacilli
Gram staining is an important differential staining technique in microbiology. Originally, Gram developed this method to differentiate pneumonia-causing bacteria in lung tissue, but today it remains the fastest, simplest, and most essential preliminary identification method in clinical microbiology. This technique uses two contrasting dyes—crystal violet and safranin—to classify bacteria into two main groups:
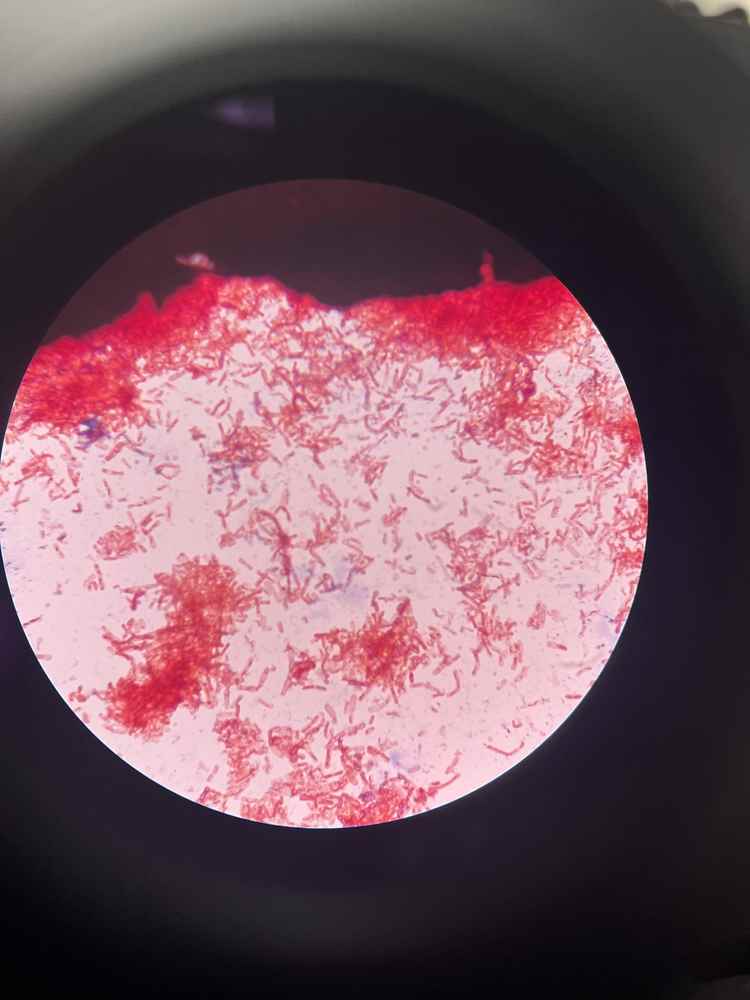
Gram-positive and Gram-negative based on cell wall structure. Gram staining allows rapid diagnosis in just a few minutes, supporting initial antibiotic selection and guiding further tests. However, the method can be affected by factors such as bacterial age (use fresh, actively growing samples), smear thickness, decolorization time, or technical errors (e.g., over-decolorization can cause false Gram-negative appearance in Gram-positive bacteria).
See also: What are Gram-positive bacilli? Structure and classification?
Clinical significance of Gram-negative bacilli
Gram-negative bacilli are a diverse group that accounts for a large proportion of community-acquired and hospital-acquired infections. They have a more complex structure than Gram-positive bacteria, with an outer LPS membrane causing high toxicity, leading to strong immune responses and common antibiotic resistance. Gram staining plays a key role in early detection, helping to classify and select appropriate antibiotics.
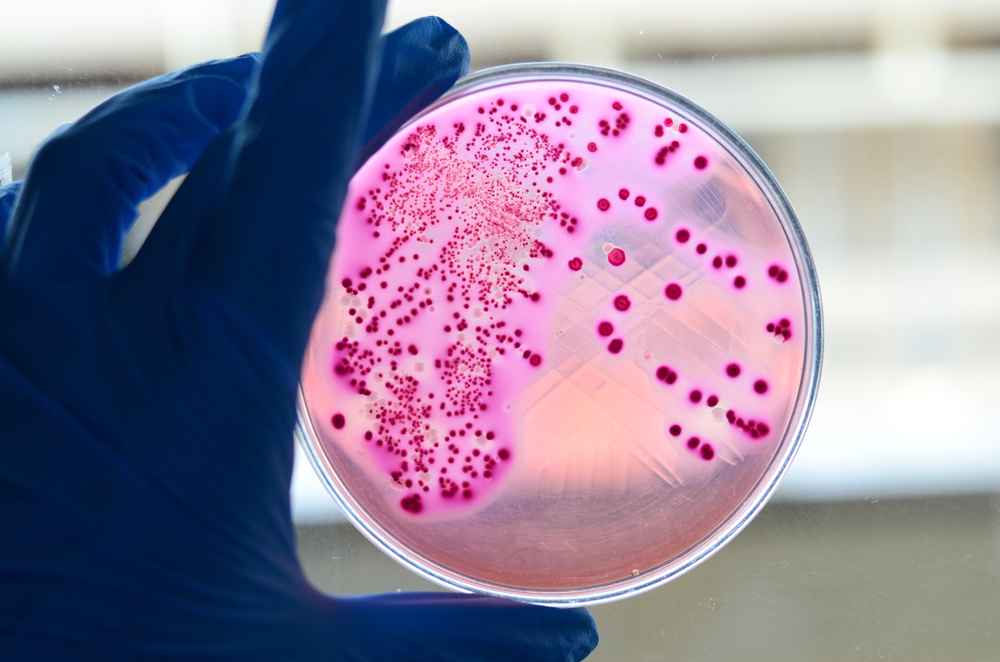
Gram staining directly from clinical specimens (sputum, urine, pus, blood, cerebrospinal fluid) helps quickly detect rod shape and Gram-negative pink/red color, supporting initial diagnosis.
Prevention of Gram-negative bacilli
- Strict hand hygiene, especially in hospitals to prevent spread.
- Infection control: Sterilize medical equipment, isolate patients with MDR organisms.
- Avoid antibiotic overuse: Use only when necessary, guided by antibiogram; implement antibiotic stewardship programs.
- Vaccination: Vaccines against Haemophilus, Neisseria meningitidis.
- Food safety: Cook thoroughly, avoid contaminated water to prevent Salmonella, Vibrio.
Gram-negative bacilli are not only rod-shaped bacteria but also represent the complexity of prokaryotic cell structure, with thin peptidoglycan and an outer LPS membrane that causes them to take up pink color in Gram staining. This explains their strong pathogenicity, difficulty in treatment, and the need for rapid diagnosis. Understanding the mechanism helps clinicians make accurate diagnoses, select appropriate antibiotics, and control infections more effectively, reducing mortality rates.


 Tiếng Việt
Tiếng Việt